The clinical efficacy of conventional radiotherapy is sometimes limited by the morphological variability of organs and anatomical structures over a multi-week treatment course. By integrating real-time imaging with high-speed computational re-optimization, ART transitions radiation oncology from a “fixed-margin” approach to a dynamic, patient-specific intervention designed to maximize the therapeutic index.
Challenges, traditional solutions and new opportunities
Adaptive radiotherapy (ART) was implemented to solve a fundamental problem in cancer treatment: the human body is dynamic, but traditional radiation plans are static.
Before ART, a patient’s treatment plan was based on a single “snapshot” (a CT scan) taken days or weeks before the first treatment. In reality, a patient’s anatomy changes every single day. ART allows clinicians to adjust the treatment plan in real-time to account for these variations.
In the case of a 5-to-7-week course of radiation, the body undergoes significant changes due to weight loss and tumor shrinkage. As a result, the skin contours can shift, and the original high-dose region might unintentionally overlap with the healthy tissue zone. Additionally, daily variations in how full the bladder or rectum are can push the target tumor out of the “crosshairs.”
Traditionally, radiation therapy professionals use “margins”—extra buffer zones of radiation around the tumor—to ensure they don’t miss the target. However, larger margins mean more damage to healthy organs (e.g., the heart, lungs, or bowel). Because ART “sees” the tumor’s exact position today, clinicians can shrink those margins, delivering a higher, more effective dose to the cancer while sparing the surrounding healthy tissue.
ART wasn’t practical until recently because the “plan–replan” cycle used to take days. Three major advancements moved it into the clinic:
- In-room Imaging: Machines like the MR-Linac and high-quality Cone Beam CT (CBCT) allow doctors to see the tumor while the patient is on the table.
- AI and Auto-contouring: AI can now outline organs in seconds, a task that used to take a physicist or doctor hours.
- Rapid Dose Calculation: High-speed computing allows the machine to generate a new, optimized treatment plan in minutes.
AI Support for Adaptive Radiotherapy Preparation
As adaptive radiotherapy moves into routine clinical use, preparation workflows must keep pace with frequent image updates and anatomical changes. AI-driven solutions can support these workflows by assisting with structure definition, dose evaluation, and data consistency when new imaging is introduced.
The four modules of MVision Workspace+®, for example, support adaptive preparation processes:
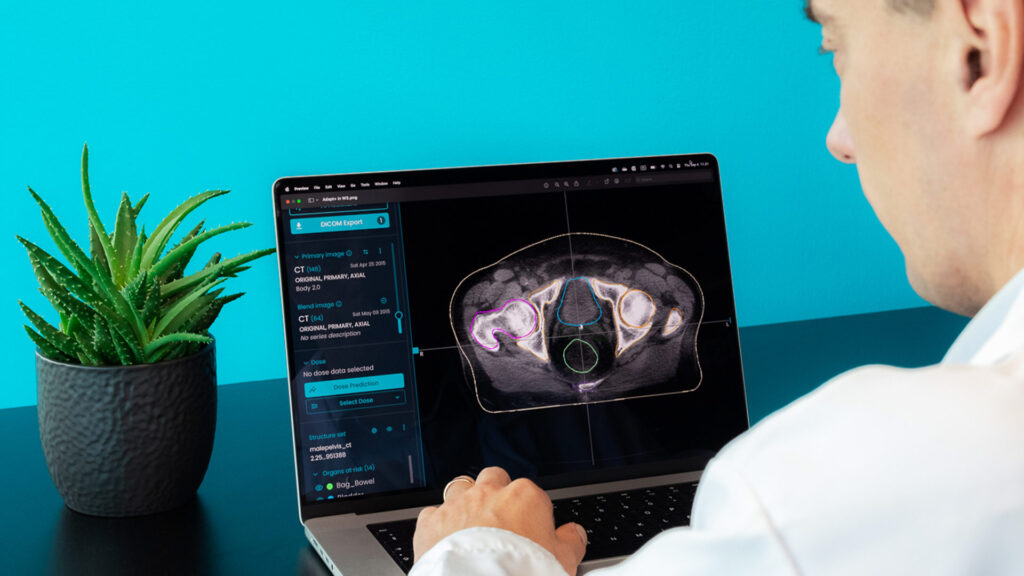
MVision Contour+® – AI-powered auto-contouring that generates guideline-based anatomical structures to support rapid contour creation from updated images.
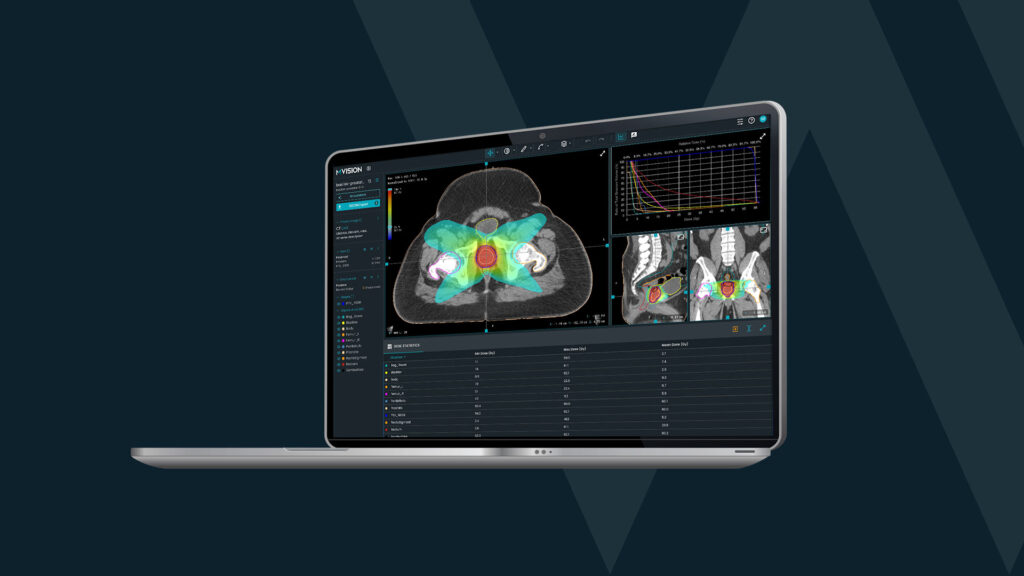
Dose+ – AI-generated dose prediction from patient-specific geometry to support evaluation and optimisation within preparation workflows.
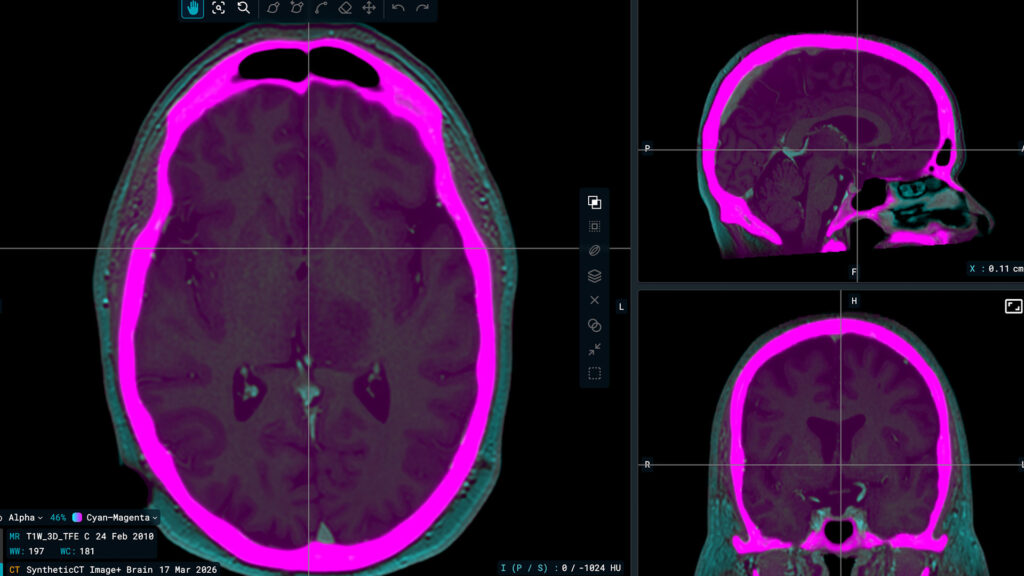
Image+ – Synthetic CT generation from MRI, CBCT, or contrast-enhanced CT to support recalculation and offline adaptive workflows.
Adapt+ – AI-assisted contour propagation across image sets to assist offline adaptive workflows when anatomy changes during the treatment course.
Together, these modules support consistent and efficient radiotherapy preparation while keeping clinicians fully in control of review and decision-making.
Online and Offline ART
The difference between online and offline comes down to one thing: Is the patient still on the treatment table while the plan is being changed?
In an online workflow, the modification happens while the patient is immobilized on the treatment couch. The clinician takes a scan, notices a change, and recalculates the dose immediately before the beam turns on. The Process involves scanning, re-contouring of the volumes of interest, re-planning, a quality check and actual treatment. It usually takes 15–30 minutes total and it’s best for organs that move or change shape rapidly from day to day (e.g., the prostate, bladder, or pancreas). The main advantage of online adaptive radiotherapy is that it offers the highest possible precision because it accounts for exactly how the patient looks right now. The disadvantage is that it requires the patient to stay still for longer and demands a high-speed team of physicists and doctors to be present.
In an offline workflow, the data is collected during that day’s treatment, but the adjustments are made later. The new plan is applied to the following sessions. The process involves analyzing scans from the last few days, identifying a trend (like significant weight loss), re-planning, and implementing the changes at a future session. It takes 24–48 hours and it’s best for gradual changes that don’t fluctuate wildly day-to-day, such as a shrinking head-and-neck tumor or a patient losing weight. It doesn’t keep the patient on the table longer and allows for a more “relaxed” peer review of the new plan. However, it cannot account for “random” daily changes, like gas in the bowel or a differently filled bladder.
Many modern clinics use a hybrid approach. They might use offline ART to adjust for the patient’s weight loss over the first three weeks, but use online ART daily to make sure they aren’t hitting the rectum while treating the prostate.
For which types of cancers is adaptive radiotherapy currently used?
If the tumor or surrounding healthy organs change position, size, or shape significantly during the course of treatment, ART can bring a dosimetric benefit.
- Genitourinary cancers represent the most common area for “online” (on-table) ART due to the high variability of daily organ filling. ART allows for “ultra-hypofractionated” prostate cancer treatments (fewer, high-dose sessions) by ensuring the beam hits the prostate and spares the rectal wall. Similarly, clinicians can create a “plan-of-the-day” that matches the bladder’s specific size at the moment of treatment. For renal (kidney) cancer, ART can be used in SBRT (Stereotactic Body Radiotherapy) to manage respiratory motion and protect the bowel.
- Gastrointestinal (GI) cancers benefit from ART implementation because GI organs (stomach, intestines) are highly sensitive to radiation and move with digestion. For pancreatic cancer, high-dose “ablative” radiation while moving the dose away from the stomach and intestines in real-time. In the case of liver cancer, adapting for breathing movements ensures that healthy liver tissue is spared, which is important especially for patients with underlying conditions, such as cirrhosis. For rectal cancer, ART is used to adapt to tumor shrinkage during treatment, potentially allowing some patients to avoid invasive surgery (the “Wait and Watch” approach).
- Head and Neck Cancers represent a classic use case for “offline” adaptive therapy. These patients often lose significant weight or experience rapid tumor shrinkage in the first few weeks. ART prevents the high-dose radiation zone from “drifting” into the parotid (salivary) glands or the spinal cord as the patient’s neck contour changes.
- Cervical and uterine cancers represent another field of use, since the uterus can tilt and shift significantly based on bladder and bowel status. Online ART (using systems like Ethos or MR-Linac) ensures the “target” is always covered without overdosing the surrounding pelvic organs.
- Radiotherapy for lung and thoracic cancers benefits from motion management technologies. For tumors that move with the patient’s breath, adaptive protocols (often involving “gating” where the beam only fires at a specific point in the breath cycle) are used to minimize damage to healthy lung tissue.
What are the practical results of implementing adaptive radiotherapy?
A recently published review on this topic concluded that multiple randomized trials are already available for offline ART. For online ART, phase 3 trials are still expected.
However, a randomized phase 2 trial of online ART for head and neck cancer showed a lower dose to the parotid gland (mean dose: 11.5 Gy vs. 16.0 Gy, p = 0.02) and lower rates of G2 or higher radiation-induced dermatitis (8% vs. 31%, p = 0.05) compared to standard radiochemotherapy. Moreover, observational studies show that online ART applied in patients with esophageal, pancreatic, rectal, and prostatic cancers are feasible and have dosimetric advantages for the organs at risk (1).
The table below summarizes some of the currently published results.
| Cancer Category | Target Volume & Setup Benefits | Organ-at-Risk (OAR) Sparing | Toxicity & Quality of Life |
|---|---|---|---|
| Cervical (2) | PTV V95% increased from 91.2% to 96.8%; average PTV volume reduced 15% by week 3. | Rectal dose decreased by 18%; Bladder dose decreased by 12%. | High target coverage (98-99%) maintained while sparing healthy tissue. |
| Head & Neck (3-5) | Tumor regression of 1.2% per day; GTV reduced to ~49% after 6 weeks; Setup error reduced from 4mm to 0.5mm. | Parotid dose reduced by 0.4–7.1 Gy; Max spinal cord dose decreased by 0.1–4.6 Gy. | Grade 2+ dermatitis reduced (8% vs 31%); improved speech, eating, and saliva production. |
| Bladder (6) | Treatment volumes reduced by 40% compared to conventional approaches. | Normal tissue volumes receiving >45 Gy reduced by 29%; >5 Gy reduced by 15%. | Significant reduction in healthy tissue irradiation. |
| Lung (7-8) | Enabled dose escalation from 66.8 Gy to 73.6 Gy via iso–mean lung dose approaches. | Healthy lung V20 reduced by 17–23% (mean 21%). | Maintains acceptable OAR doses despite higher prescription doses. |
| Rectal (9) | Maintained target coverage during tumor shrinkage. | Significant reductions in small bowel dose V15, V40, V45 and bladder dose. | Potential for "Wait and Watch" strategies due to precise adaptation. |
References
- Kalinauskaite G, Nikolaou K, Wittig A, Zips D, Zöphel K, Senger C. Online Radiotherapy: The Paradigm Shift to Real-Time Adaptive Radiotherapy. Dtsch Arztebl Int. 2025 Feb 7;122(3):59-64. doi: 10.3238/arztebl.m2024.0242. PMID: 39705230; PMCID: PMC12434711.
- Pelawi, Awan, Saufa Taslima and Elida Sihombing. “Development Of An Adaptive Radiotherapy Protocol For Cervical Cancer Patients In Medan.” Jurnal Ilmiah METADATA (2024): n. Pag.
- Schwartz DL, Garden AS, Shah SJ, et al. Adaptive radiotherapy for head and neck cancer–dosimetric results from a prospective clinical trial. Radiother Oncol. 2013;106(1):80-84. doi:10.1016/j.radonc.2012.10.010
- Castelli J, Simon A, Lafond C, et al. Adaptive radiotherapy for head and neck cancer. Acta Oncol. 2018;57(10):1284-1292. doi:10.1080/0284186X.2018.1505053
- Kataria T, Gupta D, Goyal S, et al. Clinical outcomes of adaptive radiotherapy in head and neck cancers. Br J Radiol. 2016;89(1062):20160085. doi:10.1259/bjr.20160085
- Foroudi F, Wong J, Kron T, et al. Online adaptive radiotherapy for muscle-invasive bladder cancer: results of a pilot study. Int J Radiat Oncol Biol Phys. 2011;81(3):765-771. doi:10.1016/j.ijrobp.2010.06.061
- Guckenberger M, Wilbert J, Richter A, Baier K, Flentje M. Potential of adaptive radiotherapy to escalate the radiation dose in combined radiochemotherapy for locally advanced non-small cell lung cancer. Int J Radiat Oncol Biol Phys. 2011 Mar 1;79(3):901-8. doi: 10.1016/j.ijrobp.2010.04.050. Epub 2010 Aug 12. PMID: 20708850.
- Ramsey CR, Langen KM, Kupelian PA, Scaperoth DD, Meeks SL, Mahan SL, Seibert RM. A technique for adaptive image-guided helical tomotherapy for lung cancer. Int J Radiat Oncol Biol Phys. 2006 Mar 15;64(4):1237-44. doi: 10.1016/j.ijrobp.2005.11.012. Epub 2006 Jan 30. PMID: 16446055.
- de Jong R, Visser J, Crama KF, et al. Dosimetric benefit of an adaptive treatment by means of plan selection for rectal cancer patients in both short and long course radiation therapy. Radiat Oncol. 2020;15(1):13. Published 2020 Jan 13. doi:10.1186/s13014-020-1461-3