Expert Perspectives – AI In Radiotherapy
AI in Clinical Radiotherapy: Insights from Michael Roche at CUH/UCC Cancer Centre

Could you introduce your hospital and your role there?
Cork University Hospital is a large tertiary referral centre and the main radiotherapy provider for the south of Ireland, treating approximately 2,000 patients per year across a wide range of tumour sites. The department delivers advanced techniques including stereotactic treatments and has a strong focus on service development and quality improvement.
As a Principal Physicist in Radiotherapy at the CUH/UCC Cancer Centre, I have a responsibility for advanced therapies, technology implementation, and workflow optimisation. A key part of my role involves evaluating and introducing new tools that can improve efficiency and consistency without compromising quality. This includes working closely with physicists, dosimetrists, radiation oncologists, and radiation therapists and ensuring that new technologies are integrated in a controlled, evidence-based manner within the clinical workflow.
How has AI become part of your radiotherapy workflow?
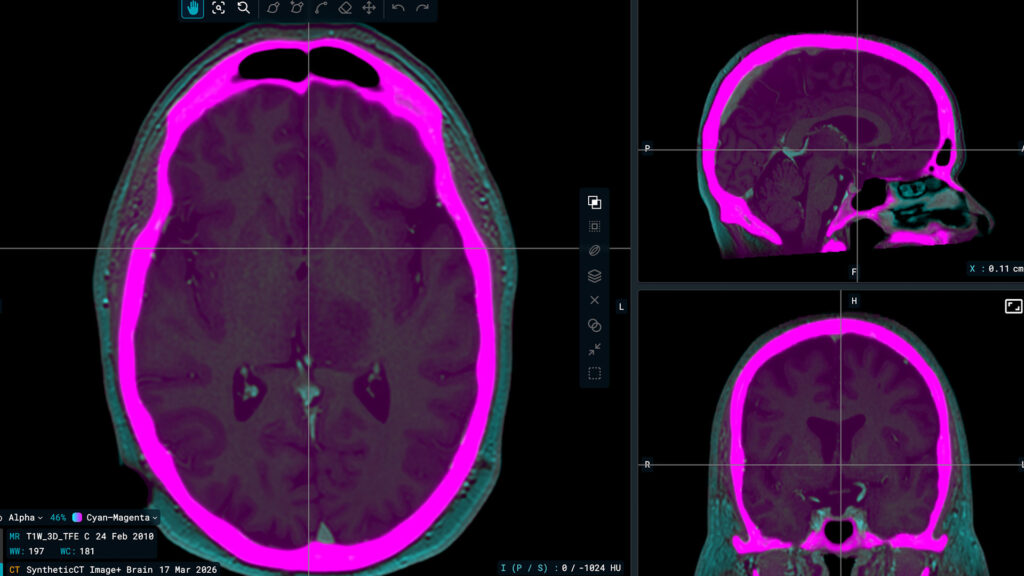
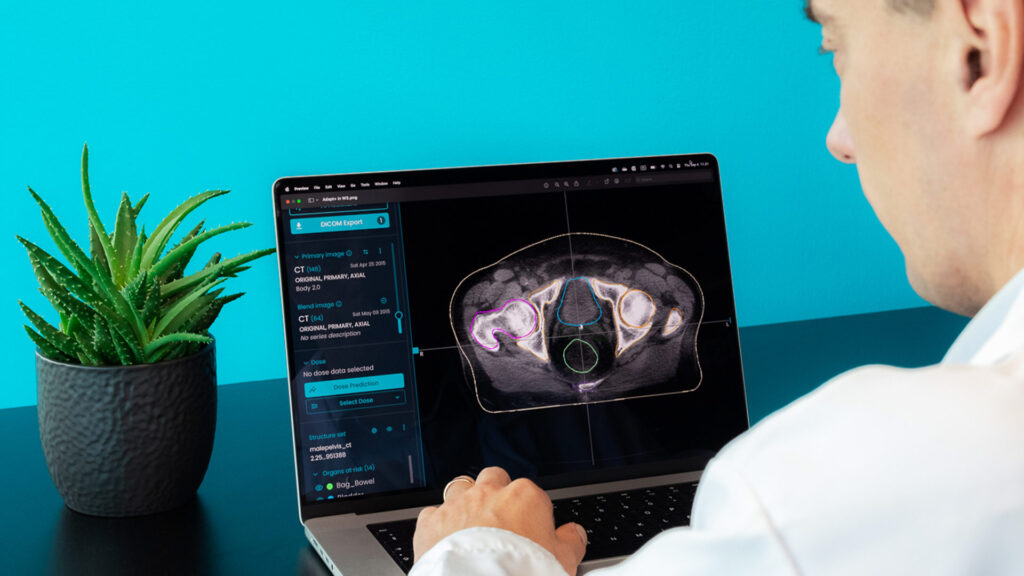
AI has become an integral part of our radiotherapy workflow primarily through its use in anatomical structure segmentation. At CUH, we introduced MVision AI Contour+ to support organ-at-risk delineation, an area that is traditionally time-intensive and variable.
Rather than replacing clinical decision-making, MVision AI Contour+ is used as a decision-support tool. The auto-generated contours provide a high-quality reference point that is reviewed, edited, and approved by the radiation oncologist. From a workflow perspective, this integration requires careful validation, staff engagement, and dynamic booking of patient start dates to take full advantage of efficiencies in the CT to treatment pathway. By embedding AI into routine practice, we’ve been able to streamline contouring timelines while maintaining clinical oversight and accountability at every step.
How have MVision AI’s solutions changed the way you work?
MVision AI’s solutions have had a measurable impact on how we manage contouring and overall workflow efficiency. By reducing the time required to reach a clinically acceptable set of contours, we’ve been able to shorten the interval from CT acquisition to treatment.
A workflow audit on the length of the CT to treatment interval for nearly 4,000 patients at CUH showed that the mean contouring workflow time and the mean CT to treatment interval reduced following implementation of MVision Contour+. We also observed a substantial reduction in contours completed outside of normal working hours, which is important for staff wellbeing and service sustainability.
From my perspective, this has shifted the focus away from repetitive manual tasks and towards quality assurance, optimisation, and clinical review. It allows healthcare professionals to spend more time on complex decision-making rather than routine contour generation.
What difference do these advancements make for your patients?
For patients, the most important impact is a more efficient and predictable pathway from initial simulation to treatment. We have found that faster contouring translates directly into shorter times to treatment planning and with optimised booking, earlier treatment start dates.
At CUH, the number of patients contoured within seven calendar days of CT increased following AI implementation, and we also observed a reduction in the time to treatment. While MVision AI Contour+ operates behind the scenes, its benefits are felt in smoother workflows and fewer delays.
Equally important is consistency. MVision AI Contour+ assisted contouring helps improve reproducibility across cases, supporting guideline-based practice. When combined with clinician review, this contributes to safe, high-quality radiotherapy delivery and a more streamlined patient experience overall.
What excites you most about the future of AI in oncology?
What excites me most is the potential for AI to support the entire radiotherapy pathway, not just individual tasks. We’re already seeing clear benefits in segmentation, but potentially the future lies in integrated systems that link contouring, planning, scheduling, and adaptive workflows.
From a physics and service-delivery perspective, AI offers an opportunity to improve consistency and capacity in increasingly busy departments. Importantly, this must be done with strong governance, transparency, and continuous evaluation.
I see AI as an enabler rather than a replacement, allowing clinicians and physicists to focus on complex cases, innovation, and patient care. As the technology matures, its success will depend on real-world clinical validation and close collaboration between vendors and clinical teams.
About the CUH/UCC Cancer Centre in Cork University Hospital
Cork University Hospital is a tertiary academic hospital and the primary radiotherapy centre for the south of Ireland. The CUH/UCC Cancer Centre delivers advanced external beam radiotherapy techniques and is actively engaged in service development, research, and the clinical implementation of innovative technologies to improve patient care. The Department of Medical Physics at the UCC/CUH Cancer Centre plays a central role in supporting safe and advanced radiotherapy delivery, with a team of physicists, dosimetrists and physics technicians providing expertise across treatment planning, quality assurance, and technology implementation.