Cancer care and radiotherapy in the US continue to face sustained demand as cancer incidence remains high across the population. According to the American Cancer Society, approximately 2.1 million new cancer cases are expected to be diagnosed in the United States in 2026 (1). Breast, lung and bronchus, prostate, and colorectal cancers together account for nearly half of all newly diagnosed cancers (2).
Radiation therapy remains a central component of cancer treatment. Large population-based analyses have consistently shown that around half of cancer patients receive radiotherapy at some point during their illness, either as a primary treatment or in combination with surgery and systemic therapies. These same analyses estimate that radiotherapy contributes to approximately 40% of curative cancer treatments, reflecting its role across many tumor types and disease stages (3).
Geographical Access to Radiotherapy
Access to radiotherapy depends not only on clinical need but also on geography. Many radiotherapy regimens require daily treatment over several weeks, making travel distance a practical barrier for some patients.
The most comprehensive national inventory of US radiotherapy facilities to date analyzed facility data through 2020. Published in the International Journal of Radiation Oncology, Biology, Physics, the study identified 2,313 radiation therapy facilities, compared with 1,987 facilities in 2005, representing a 16.4% increase over that period (4). Using population-weighted distance estimates, the authors reported that 77.9% of the US population lives within 12.5 miles of a radiation therapy facility, while 1.8% lives more than 50 miles away (4).
The study also showed that travel distance is not evenly distributed. Longer distances were associated with non-metropolitan residence, lower insurance coverage, older median population age, and lower regional income. Regions that added radiotherapy facilities over time were more likely to be urban and economically advantaged, suggesting that facility growth does not automatically reduce access gaps (4).
While no newer national facility-distance inventory has been published since this analysis, subsequent research continues to support the clinical relevance of travel burden. A 2024 systematic review examining cancer outcomes and treatment access found consistent evidence that longer travel distances are associated with differences in treatment receipt and survival across multiple cancer settings (5).
Radiation therapy facilities in the US (2020)
Of Americans live within 12.5 miles of a treatment center
Financial Burden of Cancer Care
Cancer care in the US carries a substantial economic burden that extends beyond clinical treatment alone. The National Cancer Institute’s Cancer Trends Progress Report provides a widely used national benchmark for understanding this burden. Using cancer-attributable medical services and prescription drug spending, the model estimated total cancer care costs of $190.2 billion in 2015, with projected costs of $208.9 billion under the same framework, driven primarily by population growth and aging rather than changes in treatment patterns (6).
While this model does not represent a real-time accounting of current spending, it remains an important reference point for understanding how cancer care costs scale at the national level. Within this framework, female breast, colorectal, lung, and prostate cancers, along with non-Hodgkin lymphoma, account for the largest shares of medical service costs. Prescription drug spending is highest for breast cancer, leukemia, lung cancer, and prostate cancer (6).
The report also highlights substantial variation in average annual costs by disease stage and phase of care, reinforcing how diagnosis timing and treatment intensity shape overall spending (6). Taken together, these findings continue to inform policy discussions around affordability, access, and long-term sustainability in cancer care.
New cancer cases expected in the US in 2026
National cancer care costs in 2015 (baseline benchmark)
Radiotherapy and Telemedicine
Telemedicine has become an established component of oncology care, including in radiation oncology. While in-person visits remain essential for simulation, imaging, and treatment delivery, telemedicine now supports consultations, treatment discussions, and selected follow-up visits.
Evidence for this shift has strengthened in recent years. A 2024 study published in JAMA Network Open evaluated fully remote physician management in radiation oncology across 2,817 patients. The study reported that, among 764 safety events, 763 (99.9%) did not reach patients or caused no harm, and that 97.6% of surveyed respondents rated their experience as good to very good (7).
The study also documented reductions in patient travel time and out-of-pocket expenses associated with remote care, supporting a hybrid model in which telemedicine complements, rather than replaces, in-person radiotherapy services (7). These findings reflect how telemedicine is increasingly integrated into routine radiation oncology practice rather than used only in exceptional circumstances.
Guideline-Based AI Contouring in Radiotherapy
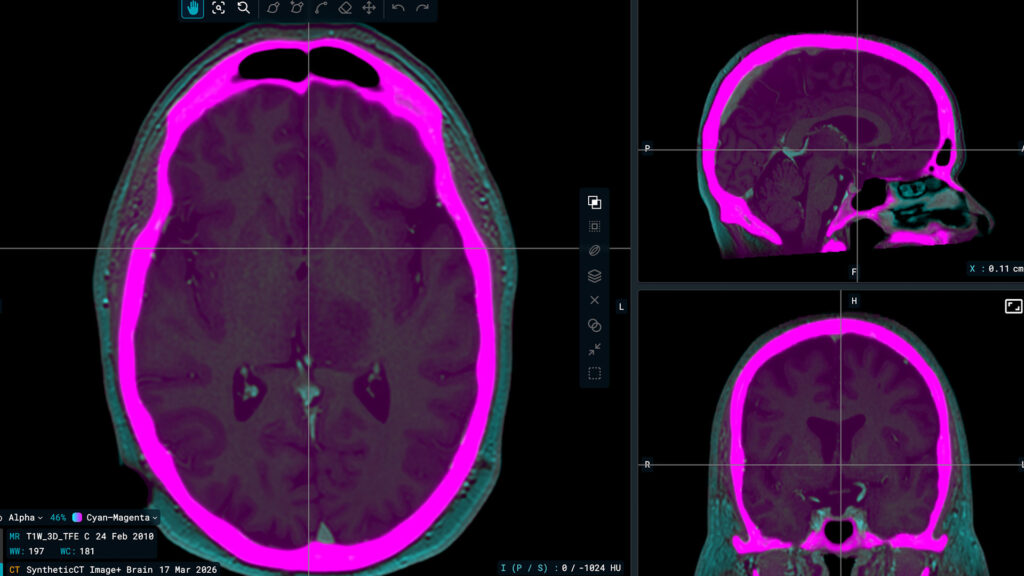
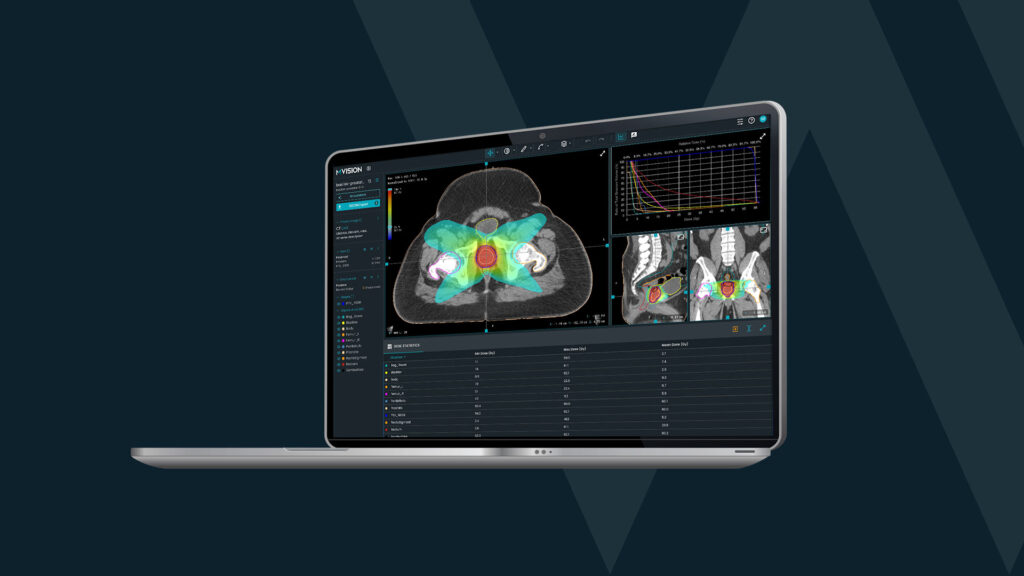
Radiotherapy planning preparation relies on accurate delineation of target volumes and organs at risk. In recent years, artificial intelligence solutions have been introduced to support this process by standardizing contouring and reducing manual workload.
For example, MVision AI’s Guideline-Based Segmentation (GBS™) provides guideline-based, AI-powered automatic segmentation for radiotherapy and is cleared by the FDA for clinical use (8). The company has also received FDA clearance for Dose+, an AI-based dose prediction tool designed to support treatment planning workflows in clinical environments (9).
These solutions are intended to assist clinicians rather than replace clinical judgment. They focus on consistency, transparency, and workflow support as radiotherapy departments manage growing case volumes.
Looking Ahead
Cancer care and radiotherapy in the US continue to advance, yet access, cost, and capacity remain persistent challenges. While technology and clinical techniques have improved, disparities related to geography and resource distribution still shape patient experience. Future progress will likely depend on how effectively health systems align infrastructure, AI, digital tools, and clinical expertise to deliver care that is both technically advanced and broadly accessible.
*This article was originally published on October 22, 2021 and has been updated to reflect current information.
References
-
- American Cancer Society. Cancer Facts & Figures 2026 (PDF).
https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2026/2026-cancer-facts-and-figures.pdf - National Cancer Institute, SEER. Common Cancer Sites.
https://seer.cancer.gov/statfacts/html/common.html - Baskar R, et al. Cancer and Radiation Therapy: Current Advances and Future Directions.
International Journal of Medical Sciences. 2012.
https://www.medsci.org/v09p0193.htm - Maroongroge S, et al. Geographic Access to Radiation Therapy Facilities in the United States.
International Journal of Radiation Oncology Biology Physics. 2022.
https://pubmed.ncbi.nlm.nih.gov/34762972/ - Silverwood SM, et al. The Relationship Between Travel Distance and Cancer Outcomes: A Systematic Review.
Advances in Radiation Oncology. 2024.
https://www.advancesradonc.org/article/S2452-1094(24)00215-X/fulltext - National Cancer Institute. Financial Burden of Cancer Care.
https://progressreport.cancer.gov/after/economic_burden - Cuaron JJ, et al. Patient Safety and Satisfaction With Fully Remote Management of Radiation Oncology Care.
JAMA Network Open. 2024.
https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2819906 - MVision AI. FDA 510(k) Clearance for Guideline-Based Segmentation.
https://mvision.ai/gbs-fda-510k-clearance/ - MVision AI. Dose+ Receives FDA 510(k) Clearance for Clinical Use in the United States.
https://mvision.ai/mvision-ais-dose-receives-fda-510k-clearance-for-clinical-use-in-the-united-states/
- American Cancer Society. Cancer Facts & Figures 2026 (PDF).