More than half a million people are diagnosed each year with esophageal cancer. It is the 8th most common cancer type and places sixth regarding mortality[1]. Several factors influence the treatment decision with this cancer diagnosis, like the stage of the disease, the tumor site, the pathological type, and the patient’s comorbidities and performance status[2].
Surgery is the preferred treatment whenever possible. However, radiotherapy is essential, especially in treating locally advanced tumors. It can be used preoperatively, combined with chemotherapy, increasing the chance of complete resection. Using adequate doses and fractionation delivered by modern radiotherapy techniques did not increase the postoperative mortality rates[3]. For the squamous cell carcinoma selected cases, radiochemotherapy (RCT) can be used as the primary treatment, keeping the surgery as a salvage option. In the case of a limited-stage disease, for patients who are unable or unwilling to receive surgery, RCT can be an alternative. For the tumors arising in the cervical region of the esophagus, RCT is preferred instead of surgery. Radiotherapy also has a role in palliative care, alleviating patients’ symptoms.
Treating esophageal cancer with radiotherapy has some challenges related to the proximity of the spinal cord, heart, and lungs. Older techniques like 2D and 3D conformal radiotherapy fail to deliver a homogenous dose to the tumor while keeping the dose received by the normal tissues at an acceptable level[4]. A comparative analysis in 676 non-randomized patients showed that IMRT was associated with better overall survival, loco-regional control, fewer cardiac deaths, and non-cancer-related deaths[5]. For preoperative simultaneous RCT, doses ranging from 41.4 to 50.5 Gy are usually prescribed. In the case of definitive RT, the dose can be increased up to 60 Gy in 1.8–2.0 Gy fractions, frequently using a simultaneously integrated boost[2].
Increased precision in treatment delivery must be supported by increased accuracy in delineating target volumes and organs at risk (OARs). For example, spinal cord contours had the higher variability in contouring thoracic organs, with a mean dice similarity coefficient (DSC) of 0.64 (range 0.2-0.82) according to an evaluation made by Global Collaborative Oncology Group (GCOG)[6]. In another study, the highest variability in target delineation in the case of definitive radiotherapy for thoracic esophageal cancer was for the nodal gross tumor volume. DSC was initially 0.37 but improved to 0.64 after the participants were instructed to follow a contouring protocol[7]. In short, the authors’ explanations for this discrepancy were the challenges of correct imaging assessment of metastatic lymph nodes in esophageal cancer and the lack of contouring protocols for these cases.
A recently published study evaluating MVision AI models showed that the median and maximum percentage of time saved for the thorax cases was 79% and 89%, respectively. The number of analyzed volumes of interest for cancers in the thoracic region was 1080, and the satisfaction grade for the automatically predicted contours was 4.86 out of 5 maximum[8].
Using AI-based segmentation decreases the inter-observer variability, providing accurate contours. As a result, patients diagnosed with esophageal cancer receiving radiotherapy can benefit from the speed and accuracy of MVision AI models.

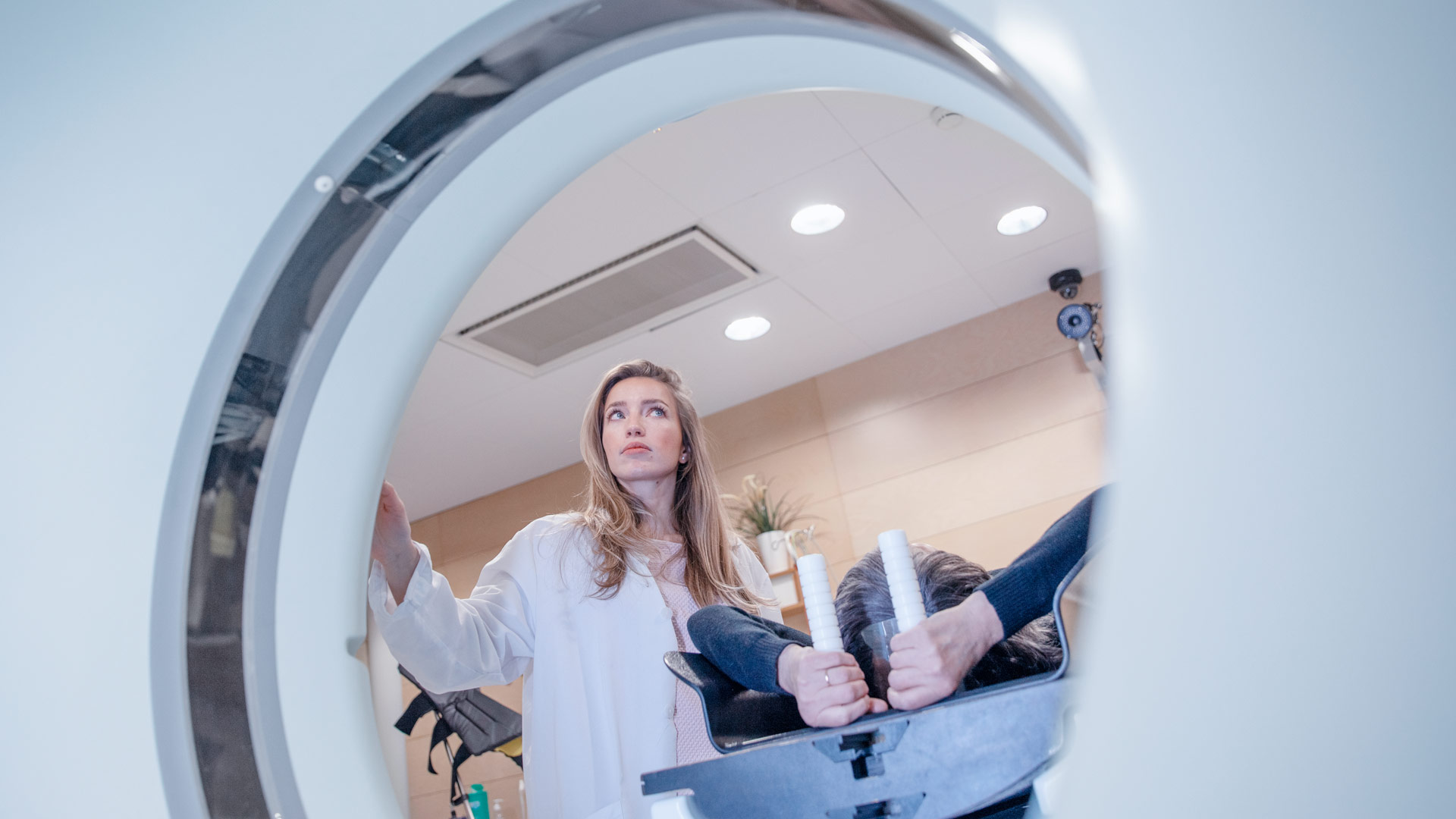
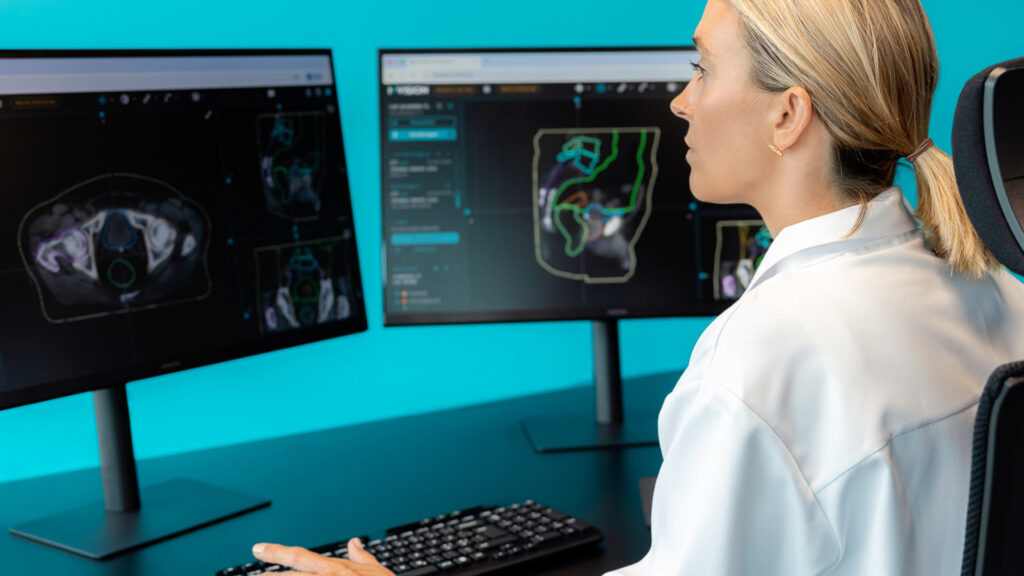
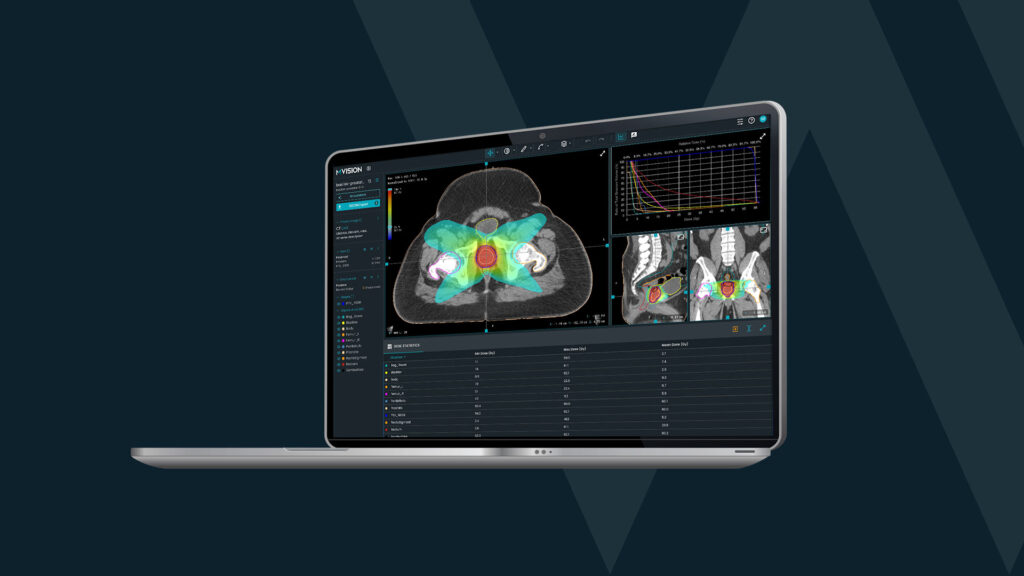
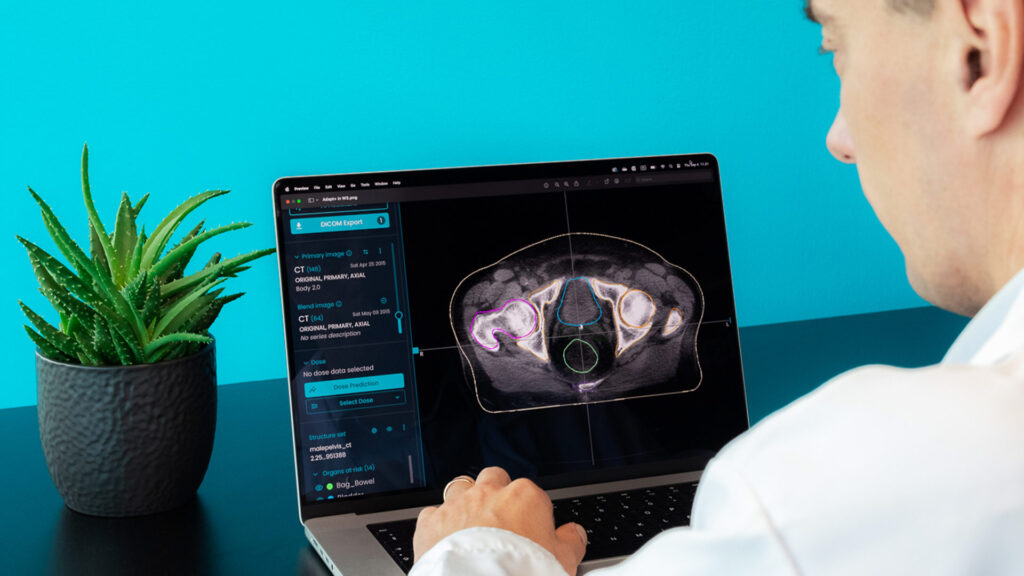
CT scan for thoracic cancer treatment with MVision’s Auto-contouring Model
References
[1] https://www.iarc.who.int/featured-news/oesophageal-cancer-awareness-month/
[2] Obermannová R, Alsina M, Cervantes A, et al. Oesophageal cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up. Ann Oncol. 2022;33(10):992-1004. doi:10.1016/j.annonc.2022.07.003
[3] van Hagen P, Hulshof MC, van Lanschot JJ, et al. Preoperative chemoradiotherapy for esophageal or junctional cancer. N Engl J Med. 2012;366(22):2074-2084. doi:10.1056/NEJMoa1112088
[4] Moon SH, Suh YG. The Role of Modern Radiotherapy Technology in the Treatment of Esophageal Cancer. Korean J Thorac Cardiovasc Surg. 2020;53(4):184-190. doi:10.5090/kjtcs.2020.53.4.184
[5] Lin SH, Wang L, Myles B, Thall PF, Hofstetter WL, Swisher SG, Ajani JA, Cox JD, Komaki R, Liao Z. Propensity score-based comparison of long-term outcomes with 3-dimensional conformal radiotherapy vs intensity-modulated radiotherapy for esophageal cancer. Int J Radiat Oncol Biol Phys. 2012 Dec 1;84(5):1078-85. doi: 10.1016/j.ijrobp.2012.02.015.
[6] J.L. Liu, X. etal. P29.03 Thoracic Organs at Risk (OARs) Contouring Variations and Consensus in Radiation Therapy for Non-Small Cell Lung Cancer, Journal of Thoracic Oncology, Volume 16, Issue 10, Supplement, 2021, Pages S1047-S1048, ISSN 1556-0864, https://doi.org/10.1016/j.jtho.2021.08.398.
[7] Chang X, Deng W, Wang X, et al. Interobserver variability in target volume delineation in definitive radiotherapy for thoracic esophageal cancer: a multi-center study from China. Radiat Oncol. 2021;16(1):102. Published 2021 Jun 9. doi:10.1186/s13014-020-01691-4
[8] Strolin S, Santoro M, Paolani G, et al. How smart is artificial intelligence in organs delineation? Testing a CE and FDA-approved Deep-Learning tool using multiple expert contours delineated on planning CT images. Front Oncol. 2023;13:1089807. Published 2023 Mar 2. doi:10.3389/fonc.2023.1089807